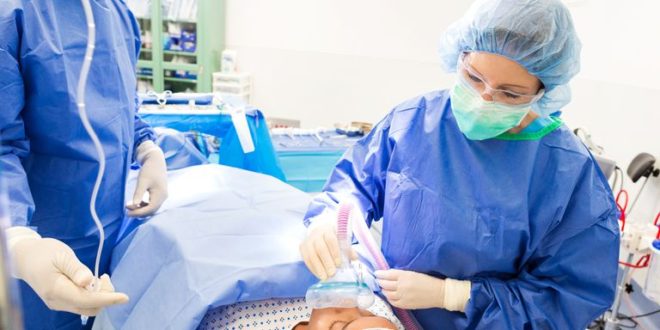
If you, or a loved one, are scheduled for surgery and you are wondering about the risks and side effects of general anesthesia, this article is for you.
You probably won’t wake up looking like this guy! And probably won’t be as awake. Though, there are things to consider about going under before the day comes.
Undergoing general anesthesia can be a source of anxiety for many people. Some of the concerns are valid; many are not.
In this post we’ll discuss these risks and side effects. While it’s not possible to include every possible side effect, we will address the most common and most serious ones.
Sore Throat
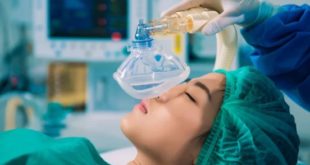
This is one of the more common side effects. While asleep, you will likely have an airway device placed to assist your breathing. Your anesthesiologist may use a LMA (laryngeal mask airway), which is a tear-drop shaped, inflatable device that sits in your throat. It has an opening that allows oxygen and anesthesia gases to flow into your windpipe and lungs as you breathe.
Alternatively, an endotracheal tube may be placed through your vocal cords and into your windpipe to more securely protect your airway (from gastric aspiration) and allow for more control of your breathing during the procedure. Your anesthesiologist will decide which device is more appropriate for you depending on your medical profile and type of surgery.
It is the placement of one of these devices that may cause you to have a sore throatonce you wake up from surgery and the device is removed.
Your throat may also feel a little scratchy if it is dry when waking up from anesthesia. This was my personal experience.
When I was still in the military, the Navy required that my wisdom teeth be removed prior to my deployment to Iraq. Because I was removing all four teeth at the same time and there was some indication that it may be a tedious and prolonged procedure, I had it done under general anesthesia (and my breathing tube was placed through my nose to give my surgeons greater room to work in my mouth).
My first memories coming out of anesthesia were in the recovery room, and I remember my throat hurting being the biggest discomfort at that time. But the reason it was so uncomfortable was that it was very dry. My surgeons most likely placed a “throat pack” to keep any bleeding from traveling further down. After this was removed at the end of the case, it left my throat feeling parched. As I woke up some more in the PACU (post anesthesia care unit), my nurse gave me some ice with which I could wet my throat and the feeling went away.
Here’s what an LMA looks like (when it’s in a good mood).
PONV (Post Operative Nausea/Vomiting)
This is one of the more common side effects of general anesthesia. There are several risk factors that make people more likely to have this bad experience.
Some of the risks are related to the patient:
- Female gender
- Younger patient
- Non-smoker
- History of Motion Sickness
- History of previous PONV
Some are related to the surgery itself:
- Longer surgery (risk goes up after about an hour)
- Surgery type: Eye, ENT (Ear, Nose, Throat), Breast, Urologic, Laparoscopic
- That list isn’t necessarily complete, even though it seems to include just about everything
Anesthesia related risk factors:
- Increased use of narcotic and anesthesia gases (inhaled anesthetics). This is sometimes unavoidable.
Have a conversation with your anesthesiologist about PONV prior to heading back for surgery, especially if you are at higher risk. There are several anti-nausea medicines that he/she may give you to combat this problem. If you are at very high risk, they may even alter their anesthetic technique.
Finally, we try to properly hydrate you during surgery through administration of IV fluids. One of the benefits is it helps with PONV. But this option may be limited depending on your medical profile (for example, we have to be careful with fluid administration in a patient with congestive heart failure, or a dialysis patient) and the type of surgery.
Post Anesthesia Confusion & Cognition
Most people wake up from anesthesia with some amount of disorientation or confusion. It takes some time for the brain to fully “wake up”, even after they regain consciousness. For most, this period lasts about 10 to 15 minutes and isn’t all that remarkable.
A smaller subset of patients may experience emergence delirium (or emergence agitation). This is described as a dissociated state of consciousness where the patient may be uncooperative or combative, often thrashing, or crying, or trying to get up and off the OR table. This is concerning because we don’t want the patient hurting themselves, others, or affecting the surgical site.
Pediatric patients and young adults are at higher risk for waking up agitated like this. Among the adults, men with military or law enforcement experience seem to be most likely to wake up in fight mode. Anecdotally, I saw more of this when I was a Navy anesthesiologist taking care of young soldiers with overseas war experience (and perhaps some underlying post traumatic stress disorder).
Most often, patients can be “talked down” as I remind them where they are, that they are waking up from surgery, and I don’t want them to hurt themselves. I also have meds available, if this is not effective and the patient’s safety is in jeopardy. I have taken some punches from patients waking up and it’s not fun (especially if they are strapping Marines), but all of us that work in this field realize it is not intentional.
An area of increasing interest and research is postoperative cognitive decline (POCD). This describes a decline in several neuropsychologic categories, such as memory, executive function, and brain processing speed. The concern is that these deficits can last days, weeks, or even longer.
There is still much research left to be done but risk seems to be higher in the elderly, those with lower education level, those with a history of previous cognitive dysfunction, and those with a history of depression or substance abuse. Interestingly, POCD does not seem to occur with higher frequency in those having general anesthesia (as opposed to other types of anesthesia). This suggests that the typical stresses of surgery, and the body’s ability to recover from that, may play a significant role here. Lots of research is still needed.
Damage to Lips or Teeth
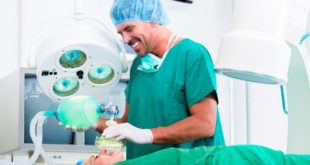
This is a very rare complication that may occur with the placement of your breathing tube. In placing this tube, once you are fully asleep, your anesthesiologist will place a laryngoscope blade in your mouth, displace your tongue and soft tissue, and visually place the breathing tube past your vocal cords and into your windpipe.
If you have more challenging anatomy, this visualization may be more difficult and increase the chances of damage. Also, make sure to tell your provider if you have any loose teeth. If dislodged, teeth can travel into your windpipe, affect your breathing, and possibly cause an infection.
Here’s what this process looks like (on a dummy, on the floor):
Reactions to Meds or Anesthetics
It’s always possible to have a reaction to any of the IV or inhaled medicines used while under anesthesia. This is why we take a detailed history of any medicines/foods/products that you are allergic to and note what types of medicines you are taking regularly (including herbal meds).
Severe, anaphylactic type reactions are pretty rare. Though we do everything possible to avoid allergic reactions, we are watching you very closely throughout your procedure and are ready to treat any adverse reaction.
End Organ Effects
This refers to the effect that anesthesia can have on all your major organs including your heart, brain, liver, and kidneys. These major types of complications such as heart attack, stroke, and yes even death, are very rare for patients that are healthy. Anesthetics can affect things like your heart rate and blood pressure, so we have standards for monitoring patients to ensure those organs are being properly perfused during surgery.
If you have significant disease in one or more of these “end organs” or if you are having a more complex surgery, your anesthesiologist may ask for more advanced studies that tell us more accurately how “healthy” those organs are.
We may also decide to place some more sophisticated monitoring. This can aid us in more closely monitoring you during surgery and even help in delivering any treatment that may be necessary (IV fluids, blood products, medication infusions, etc). These extra monitors include arterial lines, central lines, pulmonary artery catheters, and/or transesophageal echo’s. The last two are more often used in major heart or lung surgery.
We don’t take the placement of these advanced monitors lightly and only do it if they will be beneficial in taking care of you. Often, most if not all of them can be placed after you are asleep. And you will wake up with them in place.
This last part can be very scary for people to think about. But the overall take home message is that for relatively healthy people anesthesia is very safe. And the more severe complications, fortunately, are very rare.
Your anesthesiologist has gone through four years of medical school training and then four years of residency to gain the knowledge, skill, and judgement to guide you through this stressful time as safely as possible.
Now it’s your turn. Let us know what you think.
If you still have some unanswered questions on this topic, leave it in the comments section below. I’ll do my best to answer in a timely manner.
And if you’ve had anesthesia in the past, let us know what your experience was like.
Or, if you’d like to get the whole group involved, head over to the forum and post your question there. I hope this information was helpful.
We look forward to hearing from you!
Dr. Dave & Dr. Joe
 Anesthesia Myths: Get the Facts, Lose the Fear | Your #1 Anesthesia Resource in Simple language
Anesthesia Myths: Get the Facts, Lose the Fear | Your #1 Anesthesia Resource in Simple language