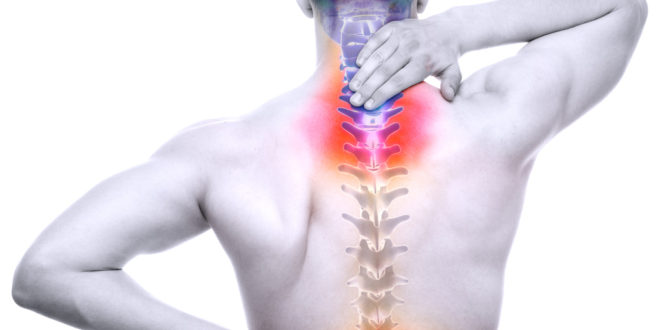
Degenerative disc disease is a common cause of back pain and/or neck pain. The location of the pain depends on the location of the problematic discs. Usually, the ones that cause pain are the lumbar discs (lower back) and the cervical ones (neck pain).
Spinal discs are the soft, compressible elements that act like a cushion between the bony vertebrae of your spine. When these discs start to break down, it can lead to pain.
This process is often a misunderstood condition.
Degenerative means that the disc’s condition typically gets worse over time. It DOES NOT mean that symptoms will necessarily get worse over time. Sometimes the back pain can actually improve with age.
Disc is pretty straight-forward. This is the “cushion-like”, cartilaginous material between the bony vertebrae of your spine. You can think of them as the shock absorbers of your spine.
Disease can also cause confusion because this is a misnomer. This is not a disease, but a condition. This degenerative condition can produce, from time to time, pain from a damaged disc.
Disc degeneration is, unfortunately, a natural part of the aging process. Over time, all of our discs undergo degenerative changes. What is different is that not everyone gets symptoms from these degenerative changes.
As we age, our discs begin to break down, or degenerate.
The discs begin to lose their natural fluid. This makes them less flexible and less able to function as shock absorbers. This also makes the disc thinner, narrowing the distance between vertebrae.
Tiny cracks and tears can also develop within the outer layer of the disc. This can cause the disc (with its soft center) to bulge, or rupture, or fragment, or lead to other problems (mentioned below).
To better understand what’s going on, we need a bit of information about the disc itself. A spinal disc is sometimes compared with a jelly donut because it has a tough, outer layer and a softer, gel-like inner layer.
Annulus Fibrosus: Tough, Outer Layer
The disc has very little nerve supply and these nerves usually penetrate only into the outer parts of the annulus fibrosus. Back pain can develop, however, if a tear in this part of the disc reaches those nerves. And with continued degeneration, those nerves can grow deeper into the disc and cause more pain.
Nucleus Pulposus: Softer, Gel-like Inner Layer
This part of the disc contains many inflammatory proteins. If they come into contact with the nerve roots of the outer layer, it will cause pain.
Keep in mind that spinal discs have a limited blood supply. This means that when injury occurs, there is a limited way in which the body can deliver oxygen and nutrients to try to repair and restore the damaged disc. This is in direct contrast to muscles, which have a much better blood supply and can heal much better.
To recap, where does pain come from in degenerative disc disease?
1. Inflammation (like the scenarios described above)
2. Micromotion Instability
What the heck is micromotion instability? When the outer parts of the disc becomes damaged, it no longer does one of its jobs very well. And that is the job of resisting motion in the spine. This is what’s referred to as “micromotion instability” because this is typically not associated with gross instability of the spine.
Both of these processes, the inflammation and micromotion instability, can result in muscular spasms of the low back. This is the body’s natural response to try to “stabilize” the area. And it can be quite painful!
A Cycle of Pain: The Degenerative Cascade
When injury occurs to a disc and the degenerative process begins, there appears to be 3 stages to this process.
1. There can be considerable pain and dysfunction caused by the acute injury.
2. There is a longer phase of relative instability at that vertebral level. The patient is susceptible to “on and off” bouts of back pain.
3. The body eventually re-stabilizes that area. The patient experiences fewer episodes of back pain.
Who is at higher risk?
Certain factors contribute to a higher risk for developing these disc problems. They include:
1. Cigarette Smoking
2. Obesity
3. Heavy-duty Physical Work (repeated, heavy lifting)
Additionally, a sudden injury (like a fall) can cause a herniated disc that accelerates this process.
So you can see how this can get a bit tricky. Pain can start after a major injury, like a car or motorcycle accident. It can start after a minor injury, like a fall from a low height. It can be triggered following a normal motion, such as bending or twisting. Or it can start gradually, without any known triggering event.
Sometimes, you can experience numbness or tingling in the arms or legs.
Making a Diagnosis
Your physician will start with a detailed and focused medical history and physical examination.
They will want to know about your symptoms, any injuries and illnesses, any activities that makes the pain worse (or better), any previous treatments and their effectiveness, etc.
During the physical exam, they’ll check the affected area for:
- Range of Motion
- Pain with movement
- Look for tender areas
- Do a neurologic exam looking for muscle weakness, numbness, tingling, and changes in reflexes
- Assess for other possibilities (infection, tumors, fractures, etc)
- Low back pain that is worse with sitting
- Lifting, Twisting, and Bending will worsen the back pain
- Walking/ Running may feel better than prolonged sitting or standing
- Changing positions frequently improves the back pain
- Lying down is usually the most comfortable position
Treatment
Conservative Options
Conservative options start with things like ice or heat to the affected area.
Medicine that is often used for temporary relief includes NonSteroidal Anti-Inflammatory Drugs (NSAIDS) such as Aspirin, Ibuprofen, and Naproxen. If these are not effective prescription medicine like oral steroids, muscle relaxants, and narcotic pain relievers may be tried.
Depending on the location and exact nature of the problem, physical therapy, chiropractic manipulation and exercises to stretch and strengthen the back may be recommended.
If the above treatments don’t provide significant relief, it may be time to consider surgical options.
Surgical Options
The 2 main surgical options are spine fusion, or artificial disc replacement.
Fusion
This is major back surgery. It involves removing the degenerated disc, decompressing any affected nerve roots, and inserting bone graft or metallic instrumentation to establish and maintain the normal disc height. This also functions to provide stability and alignment to the affected part of the spine.
As the name implies, a fusion will use bone or instrumentation to prevent movement at that spine level. With time, this may cause problems as the surrounding discs and vertebrae are placed under more stress.
This type of surgery is performed under general anesthesia. A breathing tube will be placed, and you may be positioned on your back, on your side, and/or on your abdomen. It all depends on the specifics of your injury. We’ve got several resources here that explain the anesthesia implications of this procedure.
There’s also this nice, short video by Nucleus Medical Media that uses beautiful graphics to explain the surgical procedure. It’s less than 5 minutes long.
Artificial Disc Replacement
This surgery is done through an anterior approach. For a lumbar disc, this means you will lie on your back during surgery and an incision will be made near your belly button. A general / vascular surgeon is often involved. They will help the neurosurgeon safely navigate the intestinal contents and blood vessels in your abdomen to access the spine.
Again, this procedure is done under general anesthesia.
There can be complications associated with this surgery as well. It’s beyond the scope here to cover them all, but this is a relatively new procedure (especially in the US). There isn’t as much long term data yet on how patients do with this procedure.
Which Surgery Is Better?
The potential benefits of artificial disc replacement, including limiting stress on nearby discs and retaining mobility, has to be weighed against the potential for the implant wearing out and its possible negative effects on the surrounding spinal structures.
Ultimately, a patient has to have a thorough discussion with their surgeon about all of their options, conservative and surgical, before such a decision is made. There may even be a need for a second expert opinion.
Hopefully, the information here helps you better understand degenerative disc disease and the possible treatments so that you can have a more informed and intelligent conversation with your health care providers.
 Anesthesia Myths: Get the Facts, Lose the Fear | Your #1 Anesthesia Resource in Simple language
Anesthesia Myths: Get the Facts, Lose the Fear | Your #1 Anesthesia Resource in Simple language